Abstract
The spleen is the most commonly injured organ in blunt abdominal trauma. High grade lacerations may result in severe blood loss and may be fatal if not detected early. The most common causes of blunt abdominal trauma are motor vehicle collisions, assault, and falls. Athletic injuries, while not uncommon, are very unlikely to result in major visceral blunt trauma. We present the case of a 20-year-old male who was hit by a lacrosse ball on his left flank and although the initial trauma ultrasound exam was negative, was found to have a grade IV splenic laceration on contrast CT scan. Visceral angiogram revealed no active extravasation, and the patient was managed non-operatively with close observation, serial hematocrit measurements and activity limitations. Severe splenic laceration and other visceral damage may result from lacrosse ball injury, and coaches, players and athletic medical personnel should maintain a reasonable threshold for referral to a trauma center.
Introduction
The spleen is the most frequently damaged intra-abdominal organ. 1 Splenic injuries occurring after athletic trauma constitute only a small fraction of major blunt abdominal trauma center activations. 2
However, when damage to the spleen does occur as a result of athletic trauma, it can be of great concern given the highly vascular nature of this organ. 3 Undetected, these injuries may be fatal. Coaches, athletes and athletic medical personnel should be aware of cases of severe abdominal visceral injury resulting from athletic trauma.
IRB approval for this case report was obtained at SBH Health System, Bronx, NY (IRB Number 2017.47).
Case Presentation
A 20-year-old male with no significant past medical history was brought in by EMS to the emergency department of a level 1 urban trauma center. His chief complaint was severe epigastric abdominal pain after being hit by a lacrosse ball to the left flank. Physical exam revealed an alert, hemodynamically stable male with a circular, four-centimeter diameter area of ecchymosis on the left mid-axillary line, overlying ribs nine through eleven. A focused assessment sonography for trauma (FAST) examination revealed no intra-abdominal free fluid.
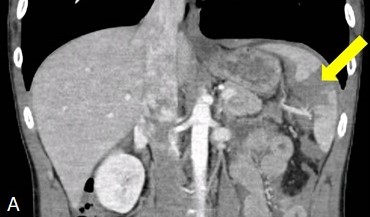
The patient experienced two episodes of blood-tinged emesis prior to computed tomography (CT) with intravenous contrast. CT scan revealed a grade IV splenic laceration of the hilum and mid-body but not involving the major splenic vasculature as well as a two-centimeter laceration of the posterior spleen with small amount of hemoperitoneum superior to the liver and in the left paracolic gutter. [fig. 1]
The patient was taken to the interventional radiology suite for formal angiogram; however, without evidence of active contrast extravasation, embolization was not indicated.
The patient was admitted to the surgical intensive care unit for close hemodynamic monitoring and pain control. Serial hemoglobin and hematocrit were stable with a hemoglobin nadir of 11.2 g/dL on hospital day two.
After the patient had been hemodynamically-stabilized, appropriate vaccinations were administered. On hospital day four, the patient was discharged home with restrictions of physical activity.
Discussion
Protected by the left lower rib cage, the spleen plays a pivotal role in both the filtration and reservation of blood, as well as immune function. Despite bony protection, the spleen remains quite vulnerable to blunt abdominal trauma across different age demographics and in both rural and urban settings. 4
Patients suffering from splenic trauma typically present with left upper quadrant pain or tenderness that may radiate to the shoulder. In the presence of hemodynamic instability, patients should receive immediate fluid resuscitation and undergo a FAST examination to guide further workup. Emergency laparotomy is reserved for persistently unstable patients with positive FAST examination.
Hemodynamically stable patients may be assessed with further imaging modalities, most commonly computed tomography. Splenic injuries are classified by CT with intravenous contrast according to grade of injury (I-V), which is based on the size, location, and if there is active contrast extravasation. 3 In our case, involvement of the hilum, thus risk for major vascular injury, led to higher grading of the splenic laceration.
The decision to treat patients with splenic injury operatively or non-operatively depends upon clinical and radiographic presentation. Operative management includes initial resuscitation, partial to total splenectomy, or angiography-guided embolization. Non-operative management includes admission to surgical intensive care unit, serial hemoglobin monitoring, and transfusions of blood and blood products as needed. 3 Within the last twenty years, non-operative management has been favored in hopes of avoiding overwhelming post-splenectomy infection (OPSI), which may have up to a 50% mortality rate. 5
Failure of non-operative management of splenic laceration is seen more frequently in higher grade injuries, higher injury severity score, hemoperitoneum, and polytrauma. 3 Our patient had a high-grade injury based on location of the laceration, but due to hemodynamic stability and lack of contrast extravasation was appropriate for trial of non-operative management.
Athletic trauma-related major abdominal visceral is uncommon. One case report cited two instances of splenic injury resulting from goalie collision with a soccer ball. 6 Similarly, a recent case report documented splenic laceration, intraparenchymal hematoma, subscapular hematoma, and hemoperitoneum after being hit in the abdomen by an icy snowball during a snowball fight; detection of massive hemoperitoneum resulted in emergency splenectomy. 7
In an epidemiologic review of injuries sustained by NCAA lacrosse players, musculoskeletal injuries and concussions are most common with no visceral injuries noted. 8 Our extensive literature review revealed only one other case of injury to the spleen induced by a lacrosse ball. Dating back to 1999, this case report described lacrosse ball trauma as an unprecedented mechanism of splenic injury. Detection of a grade IV splenic laceration with massive hemoperitoneum resulted in emergency splenectomy. 9
To our knowledge, our case is the second report of lacrosse ball-related splenic laceration and the first to be managed with a modern non-operative algorithm.
These case reports serve as a collective reminder of why coaches, players and athletic medical personnel must be adept at recognizing unusual presentations and rare causes of splenic laceration.
Conflict of Interest: The authors declare no conflict of interest.
This paper was presented as a poster presentation at the 2017 Residency Research Day at SBH Health System, Bronx, NY in May of 2017.
Figures
References
-
Poletti PA, Mirvis SE, Shanmuganathan K, Takada T, Killeen KL, Perlmutter D, et al. Blunt abdominal trauma patients: can organ injury be excluded without performing computed tomography? J Trauma. 2004;57:1072–81.
-
Smith J, Caldwell E, D’Amours S, Jalaludin B, Sugrue M. Abdominal trauma: a disease in evolution. ANZ J Surg. 2005;75:790-4.
-
Forsythe RM, Harbrecht BG, Peitzman AB. Blunt Splenic Trauma, Scandinavian Journal of Surgery. 2006;93: 146-151
-
Bjerke, HS. (2017, April 3). Trauma: Splenic Rupture. Medscape. Retrieved 4/16/2017 from http://emedicine.medscape.com/article/432823-overview#a4.
-
Gannon EH, Howard T. Splenic injuries in athletes: a review. Curr. Sports Med. Rep. 2010;9:111-4.
-
Padlipsky PS, Brindis S, Young KD. Splenic injury after blunt abdominal trauma during a soccer (football) game. Pediatr Emerg Care. 2014;30:725-9.
-
Buskova J, Polackova MJ, Pavlovsky Z. Snowball fight: an unusual cause of spleen injury. Soud Lek. 2017;62:6-7.
-
Kerr ZY, Quigley A, Yeargin SW, Lincoln AE, Mensch J, Caswell SV, et al. The epidemiology of NCAA men’s lacrosse injuries, 2009/10-2014/15 academic years. Injury Epidemiology. 2017;4:6
-
Gangemi JJ, Binns OA, Young JS. Splenic injury after athletic trauma: a case report of splenic rupture induced by a lacrosse ball. J Trauma. 1999;46:736-737.