Introduction
As the pandemic caused by the novel coronavirus SARS-COV-2 spreads worldwide, there are increasing concerns regarding the allocation of the available resources in order to control its impact. Given the limited number of test kits in the United States, many health care systems initially considered Covid-19 infection as a diagnosis of exclusion, only testing after ruling out other possible pathogens. We report a case of coinfection of SARS-COV-2 and Influenza B. This case emphasizes the need for SARS-COV-2 testing despite a positive screening test for other viruses. Every effort should be made to ensure early detection of the cases in order to implement adequate measures to prevent the spread of the disease.
Case Presentation
On March 16, 2020, an 81-year-old female presented to an urgent care clinic in the Bronx, New York, complaining of shortness of breath, subjective fever, chest tightness, and persistent cough. The patient had a past medical history of COPD (on home oxygen), pulmonary hypertension, breast cancer on remission, hypertension, hyperlipidemia, and diabetes mellitus. She was a former smoker. The patient denied recent sick contacts or recent travels. She stated that her symptoms started two days prior to her urgent care visit.
During the initial evaluation, the patient was found to have marked tachypnea and hypoxemia with an oxygen saturation of 84% on room air. She was then transferred to the hospital. At triage in the emergency room, she presented a temperature of 99.3 ºF, a blood pressure of 210/120 mmHg, a respiratory rate of 26 breaths per minute; and a pulse of 94 beats per minute. Oxygen saturation was 85% on room air. After an initial evaluation, she was placed in a special unit deployed for possible Covid-19 cases.
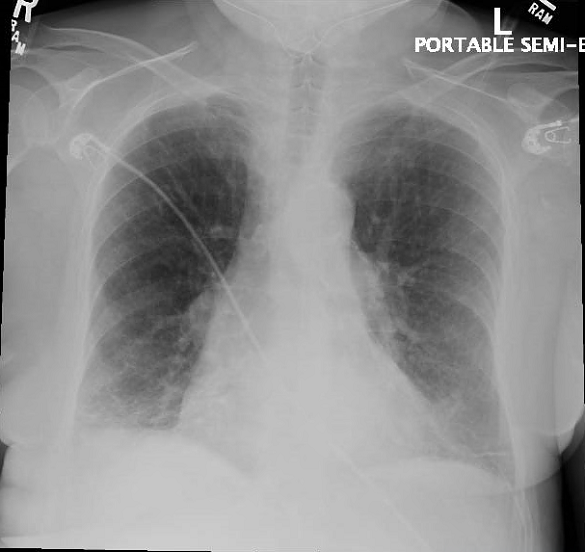
On physical examination, lung auscultation revealed bilateral rhonchi and decreased breath sounds in the lung bases. A chest radiograph showed mild pulmonary vascular congestion, vague patchy bibasilar airspace opacities and a small right pleural effusion (Image 1).
[fig. 1]
An initial venous blood gas on an FIO2 of 32% was consistent with hypercapnia (PCO2 55.7), pH of 7.34, and partial pressure of oxygen of 29.0.
A nasopharyngeal swab sent for rapid Influenza testing was positive for Influenza B by nucleic acid amplification. Initial workup included a CBC that showed a white blood cell count of 7.5 10*3/uL with lymphopenia and hemoglobin of 14.4. The initial troponin was negative. EKG was unremarkable. BNP level was 217 (Table 1).
The patient was admitted to the general medical floor under the impression of Influenza, possible community-acquired pneumonia versus COPD exacerbation, and possible Covid-19; and was started on Oseltamivir, albuterol, ceftriaxone, and azithromycin. She was admitted to an isolation room on contact and airborne precautions due to concerns for Covid-19.
Given the patient´s comorbidities, initial X-ray findings, and lymphopenia, in the setting of an increased number of cases in the community during the same period of time, the decision was made to test for SARS-COV-2. Nasopharyngeal and oropharyngeal swabs were performed via nucleic acid amplification using the cobas(R) SARS-CoV-2 test. This test was performed by LabCorp Laboratories. The test was positive and reported on March 18th.
During the first three days of admission, the patient did not show improvement in her symptoms. She complained of shortness of breath, experienced several episodes of fever (101 ºF), cough and tachycardia. She required between 3 to 4 liters of oxygen supplementation.
When the diagnosis of Covid-19 was established and the patient showed no signs of improvement, she was started on Lopinavir/Ritonavir and hydroxychloroquine. The patient received supportive therapy with acetaminophen and ondansetron as well as her regular medications: albuterol, amlodipine, roflumilast, simvastatin and exemestane. She was continued on oseltamivir and ceftriaxone. Azithromycin was switched to doxycycline due to prolonged QTC.
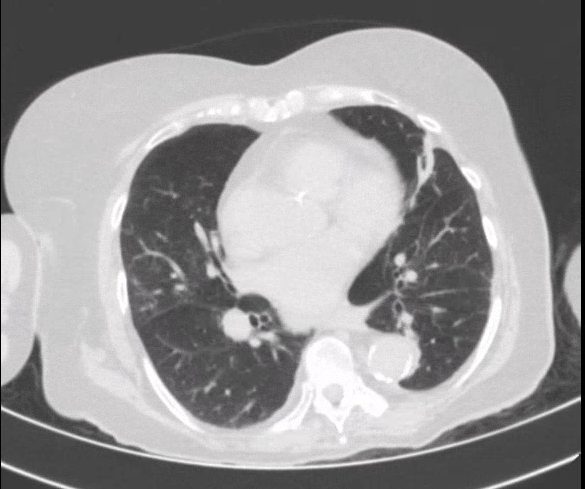
Computerized tomography of the chest was performed on March 18th and evidenced mild consolidation anteriorly and posteriorly in the lung bases bilaterally (Image 2). [fig. 2]
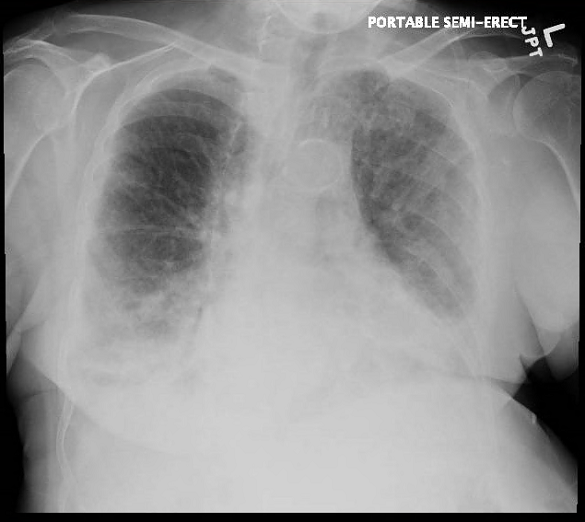
During the next three days, the patient developed worsening respiratory distress and required a higher amount of oxygen supplementation. A repeated chest Xray showed worsening bilateral infiltrates (Image 3).
[fig. 3]
Vancomycin was added due to concerns of superimposed bacterial infection. Respiratory status worsened and on March 22nd, the patient had a saturation of 83% on 10 liters of oxygen via a nonrebreather mask. After a discussion with next of kin, DNI/DNR orders were placed. The patient expired on March 24th.
Since the detection of the first case, our health care system is now testing for both SARS-COV-2, Influenza and other viral pathogens simultaneously. Within 48 hours, three other cases of SARS-COV-2 and Influenza coinfection have been detected.
Discussion
As of March 30, 2020, a total of more than 700,000 cases of Covid-19 have been confirmed worldwide during the current outbreak. 1 Because of limitations in the availability of test kits at the beginning of the Covid-19 pandemic, patients were initially being screened for other etiologies of respiratory tract infections by PCR tests including influenza, before being tested for Covid-19. Despite enormous efforts to overcome the shortage of testing in the United States, the available number of test kits at this moment is not enough to meet the current demands.
A report from Stanford Medicine Data Scientists showed that 22.4% of the patients with Covid-19 had also positive results for other viral pathogens. 2
Coinfection of SARS-CoV-2 and influenza is a challenge that health care providers are facing during the current pandemic. 3 As of March 15, 2020, CDC estimates that there have been at least 38 million flu illnesses, with 390,000 hospitalizations and a total of 23,000 deaths from flu. 4 Our case highlights a probably overlooked situation during the current pandemic where a single patient presents with coinfection with two common pathogens. Our case report illustrates the importance of testing for both influenza and SARS-COV-2.
Diagnosis of Covid-19 is challenging during the influenza season as it is difficult to differentiate upper respiratory infections due to SARS-COV-2 from influenza. Influenza and other respiratory viruses share very similar clinical characteristics such as fever, cough, and shortness of breath.
Conclusion
In summary, our case illustrates patients are being coinfected with both Influenza and SARS-COV-2. This suggest that the algorithm for screening for common pathogens before testing for SARS-COV-2 should be discouraged. Given the possibility of two simultaneous infections, Covid-19 should not be a diagnose of exclusion. Due to overlapping symptoms of influenza and the novel coronavirus, SARS-COV-2 and influenza should be simultaneously tested in patients who are admitted to the hospital. Adequate testing availability is required in order to prevent the spread and the burden of the disease.
References
-
Nigam Shah. Higher co-infection rates in COVID19.
https://medium.com/@nigam/higher-co-infection-rates-in-covid19-b24965088333 -
Wu X, Cai Y, Huang X, Yu X, Zhao L, Wang F, et al. Co-infection with SARS-CoV-2 and Influenza A Virus in Patient with Pneumonia, China. Emerg Infect Dis. 2020:26 doi: 10.3201/eid2606.200299. [Epub ahead of print]
-
Weekly U.S. Influenza Surveillance Report, March 14- March 21, 2020.
https://www.cdc.gov/flu/weekly/index.htm
Table 1
Clinical laboratory results
| Measure | Reference range | Illness day 3. Admission day 1.
3/16/20 |
Illness day 5.
Admission day 3. 3/18/20 |
Illness day 6.
Admission day 4. 3/19/20 |
Illness day 7
Admission day 5. 3/20/20 |
| White blood cell count | 4-10 10*3/uL | 7.5 | 9.8 | 7.1 | 6.9 |
| Red blood cell count | 3.93-5.22 10*6/ul | 5.5 | 4.97 | 4.64 | 4.98 |
| Absolute neutrophil count | 1.56-6.13 10*3/uL | 5.89 | 8.63 | 6.07 | 5.58 |
| Absolute lymphocyte count | 1.18-3.74 10*3/uL | 0.86 | 0.63 | 0.59 | 0.59 |
| Platelet count | 182-369 10*3/ul | 192 | 195 | 179 | 161 |
| Hemoglobin | 11.2-15.7 gm/dl | 14.4 | 13.7 | 12.6 | 13.5 |
| Sodium | 135-145 mEq/l | 134 | 139 | 141 | |
| Potassium | 3.5-5.3 mEq/L | 3.4 | 4.2 | 4.2 | |
| Chloride | 96-108 mEq/L | 97 | 104 | 103 | |
| Glucose | 70-99 mg/dl | 99 | 91 | 107 | |
| BUN | 8-23 mg/dl | 13 | 30 | 27 | |
| Creatinine | 0.6-1.2 mg/dl | 1.0 | 1.0 | 1.1 | |
| Albumin | 3.8-5.0 mg/dl | 4.4 | 3.3 | 3.4 | |
| Alanine aminotransferase | 4-36 IU/L | 13 | 12 | 15 | |
| Arginine aminotransferase | 8-33 IU/L | 27 | 28 | 38 | |
| LDH | 100-190 IU/L | 123 | 264 | ||
| CPK | 26-140 IU/L | 125 | |||
| Troponin | 0.00-0.49 ng/L | 0.09 |